Dynamics of FUE
Anatomical Considerations

Anchor system
This complex system consists of multiple structures that hold the follicular group within the surrounding tissues. The anchoring system includes the epithelium and superficial dermis that surround the follicles, a sebaceous gland, the insertion of the arrector pili muscle, the connections between the CTS and the surrounding connective tissue.
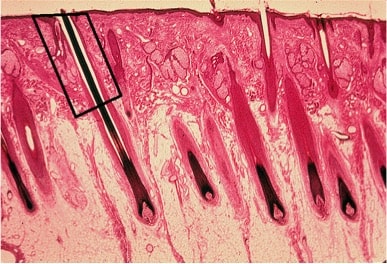 The initial incision or scoring should be able to release the graft from its anchor system. That allows an easy and minimally traumatic extraction of the graft. The depth of the initial incision or scoring by convention, begins at 2.5mm. For scalp hair, the range varies between a very shallow 1.2mm to a maximum depth of 3.5mm. Adjustments are made during the graft testing phase which is crucial in obtaining optimal results as even a minimal alteration (as small as 0.1mm), can result in grafts appearing depressed, rotated or lost in the shaft of the punch.
The initial incision or scoring should be able to release the graft from its anchor system. That allows an easy and minimally traumatic extraction of the graft. The depth of the initial incision or scoring by convention, begins at 2.5mm. For scalp hair, the range varies between a very shallow 1.2mm to a maximum depth of 3.5mm. Adjustments are made during the graft testing phase which is crucial in obtaining optimal results as even a minimal alteration (as small as 0.1mm), can result in grafts appearing depressed, rotated or lost in the shaft of the punch.
Splay
 Follicles within each follicular unit don’t always follow the same path along the entire length of their grouping. The upper portion of the follicular unit usually sits in a tightly bound bundle. Once beyond the bundle, the lower portion of the follicular unit rests more freely within the tissue. At the very distal aspect which encompasses the dermal papilla, the individual hair follicles usually separate from each other. This unbound nature of the terminal region results in an outward splay of the bulb within the surrounding fat of deeper layers of the skin.
Follicles within each follicular unit don’t always follow the same path along the entire length of their grouping. The upper portion of the follicular unit usually sits in a tightly bound bundle. Once beyond the bundle, the lower portion of the follicular unit rests more freely within the tissue. At the very distal aspect which encompasses the dermal papilla, the individual hair follicles usually separate from each other. This unbound nature of the terminal region results in an outward splay of the bulb within the surrounding fat of deeper layers of the skin.
The splay of hair follicles is as important as the exit angles. Because the hair follicles splay at the deeper levels, it is less likely that all will fit into the extracting punch. This crowding superficially followed by distal outward splay may increase the risk of transection of hair follicle. Fortunately, the percentage of follicular units exhibiting significant splay is minimal as most hair follicles usually follow the same direction within their grouping as they dive deeper into the tissue. During manual FUE scoring, consideration is given to the minimal depth necessary to liberate the grafts from the anchor system.
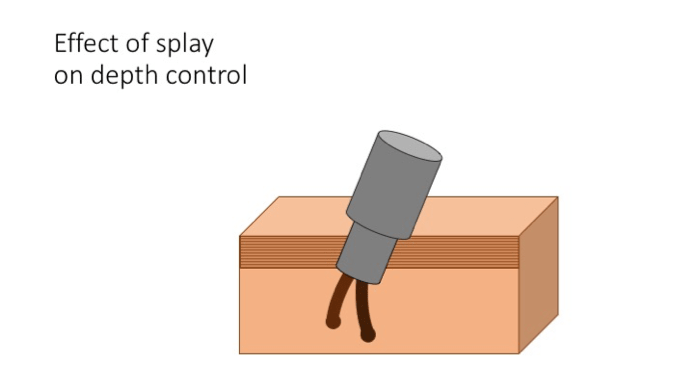
Effect of splay on depth control – To avoid the pitfall of injury to the graft, refinement of the depth of the excision is made by adjusting the depth control. Through the technique of graft testing, the depth control is tuned to the optimal depth to allow dislodgement of the anchoring system yet guard against overshooting depth resulting in transection.
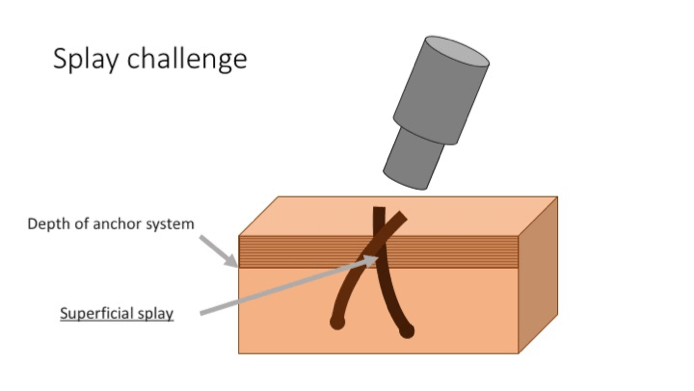
Splay Challenge – The challenge is when the splay occurs more superficially within or in close proximity to the anchor system. When presented with this situation, we cut through the anchor system by slightly increasing the scoring punch length which invariably increases the transection rate.
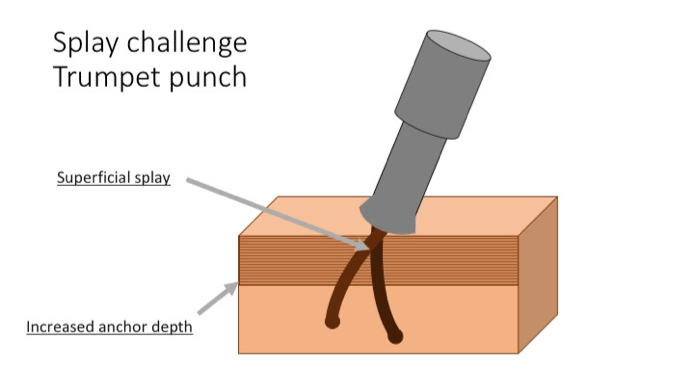
Solution – To remedy to the high transection which results when the anchor system is too deep or when the splay starts too superficially is to either increase the size of the punch or minimizing the sharpness of the contact points of the punch. Invariably, increasing the size of the punch will enlarge the wound surface area while it may only minimally reduce the transection rate.
In contrast, reducing the sharpness of the punch contact point can successfully reduce the transection rate in most cases. Thus, the effects of a sharp punch edge on the follicles is thereby eliminated. One solution put forth is the two-step extraction model which utilizes a sharp edge to initially score the skin and a blunt edge to advance the dissection deeper. A working example of this duel cutting edge method is the basis of the ARTAS system which artfully executes this punch within a punch technology. The Safe system by comparison uses a rotating blunt punch tip as its cutting edge to minimize transection rate. The remaining option to avoid cutting the follicles with a sharp edge is to switch to a flat or trumpet punch. Trumpet punches have a beveled sharp edge facing away from the center. A flat punch helps minimize the transection rate by creating a nominal deviation from the central axis of follicular unit. This edge is instrumental in reducing the transection rate especially when the operator choses to increase the scoring depth to counteract the effect of an exaggerated splay.
Skin Immobilization
Crucial for the execution and continued successful extraction of grafts, immobilization of the skin is imperative. A controlled setting of multi directional tension is applied to stabilize the donor skin for precise extraction of the grafts. There are several methods to provide the necessary traction. During a single case, a combination of methods may be utilized to facilitate grafts extraction
- Three-point traction by scorer (single person) – While using the punch device 1st and 2nd fingers of the opposite hand pull against each other and against portions of the hand that holds the punch. This creates a 3-point traction in close proximity to where the operator is scoring. This method requires a certain amount of manual dexterity but if done properly it is one of the most effective methods of skin immobilization.
- Two-point traction (2 person) – The opposite hand of the operator provides upper traction while an assistant provides a point of traction below but in close proximity to the punch.
- Three-point traction (2 person) – In addition to the operator’s single hand traction, two other hands can provide traction in opposing directions thus creating the taut field of a three-point traction.
- Tumescent effect – Superficial infiltration of the dermis with saline, (with and without epinephrine), provides the best traction of the scalp. The tension of the tumescent effect lingers only for a short time before the fluid dissipates into the interstitial space. Infiltration should transpire in an organized stepwise fashion while moving across the donor area. Small boxes should be outlined with a marking pen as infiltration of fluid provides the necessary tension for scoring within the box.
Punch Set Up
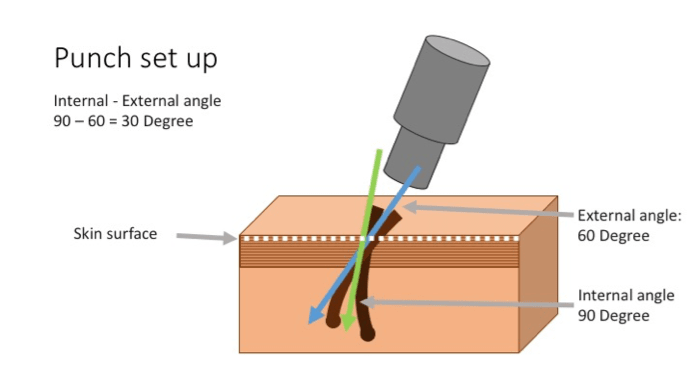
- Internal – External Angle – It may or may not be different and can be found by adjusting the angle based upon the transection angles. This angle varies depending on the extraction location within the donor region. It is noted that there likely will be a noticeable difference in the external/internal angle of hair shafts. Observing the external/internal angle difference in different areas, there is only a negligible difference in the external and internal angle of hairs in the temporal areas. In contrast, when approaching the midline of the permanent zone of scalp this angle difference become more exaggerated. That means, the internal angle of the hair follicle becomes closer to the vertical axis. This difference in angle based on the location of the donor hair should be taken into consideration when scoring each and every graft. This individual variable can only be reckoned with by the operator making the necessary adjustments using the graft transection angles as a guide.
- Initial approach –
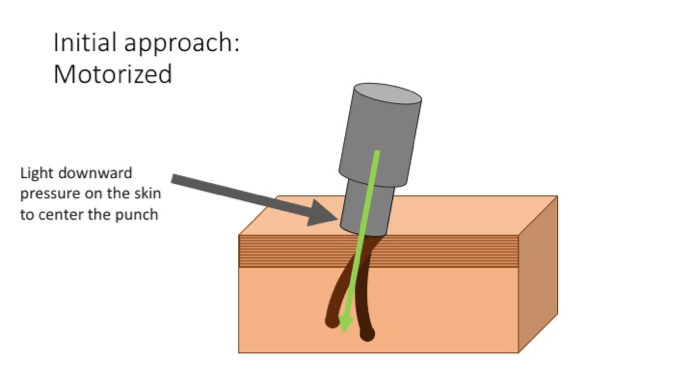
- Motorized (Off center) – During motorized scoring often the initial approach of the punch is off center when aligning the punch over the follicular units. Subsequently, during the next step of the cutting maneuver, there is light downward pressure on the skin which results in the shaft(s) becoming centralized within the punch.
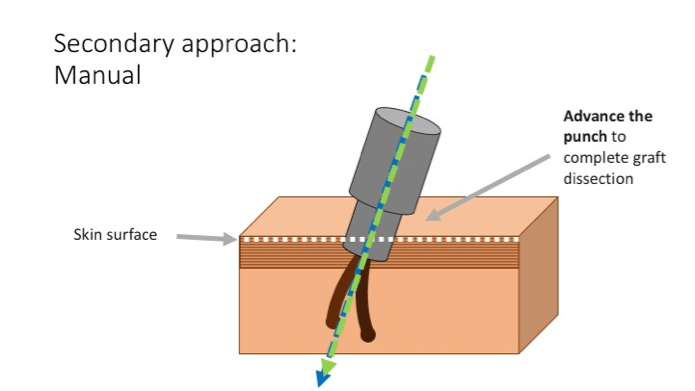
- Manual non-motorized (Centered) – The approach is different when performing this by the non-motorized manual punches. The hair shaft must be centered at the onset, as the punch is held perpendicular to the skin for the initial scoring. The angle of the trocar then changes during the follow through to accommodate the exit angle and allow the shaft(s) to remain centralized as it is advanced.

- Motorized (Off center) – During motorized scoring often the initial approach of the punch is off center when aligning the punch over the follicular units. Subsequently, during the next step of the cutting maneuver, there is light downward pressure on the skin which results in the shaft(s) becoming centralized within the punch.
- Pause (then go technique) – During motorized scoring, pause the punch tip initially as it touches the skin surface to allow for the engagement of the tip. This split-second pause enables the upper rim of the sharp punch to bury itself and essentially disappear into the skin. In other words, the pause allows for the skin surface to be completely cut circumferentially before the punch is further advanced.
- Advancing the punch – The final step is a quick advancement of the punch to complete the scoring of the graft through the anchoring system. This step should be done quickly and effortlessly but only if the prior stage s is done correctly. There should not be much resistance in advancing the punch since the toughest layers of scalp are located on the very top 2-3mm of skin. A speedy advancement of the punch minimizes the contact time of the cutting edge alongside the follicles which can translate into a lower follicular transection rate.
- Depth control – Anchor system is only limited to the upper 1-3 mm of follicles in most cases. Anchor system should be cut through in order to be able to extract the grafts effortlessly. When using a sharp punch we have to minimize the depth of our cut to minimize the chance of transecting the follicles. Dull punches as in ARTAS robotic approach can be advanced to the entire length of follicles. Using a sharp punch, any splay in grafts or any angle change brings us cutting edge in touch with the follicles and can lead to partial of completed transection. Limiting the punch depth helps cut through anchor system without unnecessarily increasing the risk of transecting the grafts.
Testing Graft Qualities
To ensure optimal graft quality, it is mandatory to test the grafts as you initially harvest. Thereafter, periodic testing of grafts is necessary to safeguard quality. Maintenance of quality is done in a stepwise fashion.
- One at a time – In the beginning, grafts should be extracted one at a time. During graft testing, information regarding proper depth, external/internal angles and splay is gathered by the operator. Slight adjustments are made with each graft that is removed. This testing period all be it time consuming, is a valuable and necessary step as it essentially sets the parameters for a smooth rest of the day.
- Three at a time– Once satisfied with the appearance of the grafts obtained one by one, the operator can increase the pace and score “three at a time”. Fine-tuning while moving faster until the normal speed of the extraction is reached.
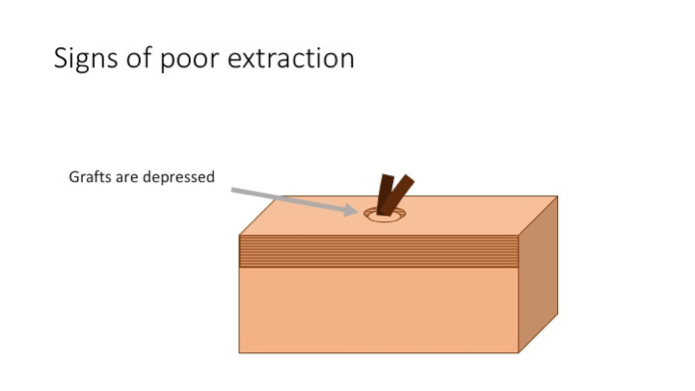
- Testing while extracting with no interruption to observe the grafts. It is advisable that a technician periodically check the last few grafts scored especially in a zone of transition. This is particularly important if there is a significant distance (of greater than 2 inches), between the surgeon and the extracting technician. Grafts should be deftly displayed to the surgeon for quick viewing essentially without disruption of the scoring process. Periodic testing helps detect any subtle changes that may occur from one area to another. Testing should be done expeditiously particularly if the surgeon notes any signs of poor extraction. Signs of poor extractions are:
- Grafts not elevated properly or appear depressed
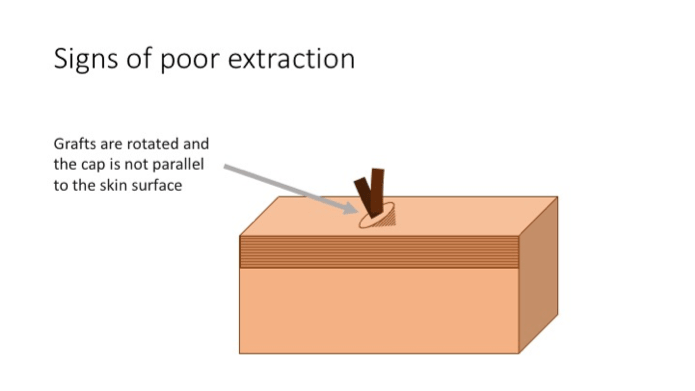
- Grafts are rotated and skin cap is not parallel to the scalp
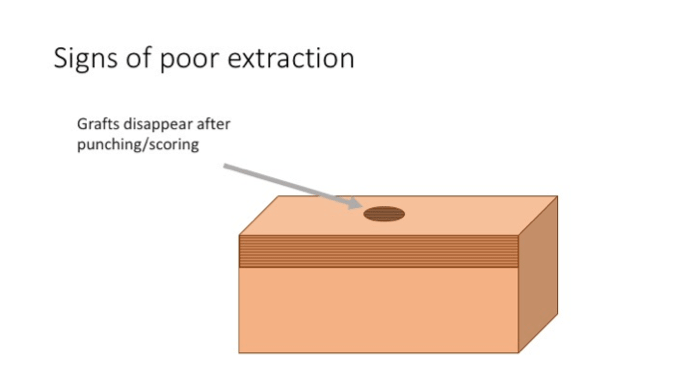
- Grafts disappear after punching/scoring
Signs of Good Extractions
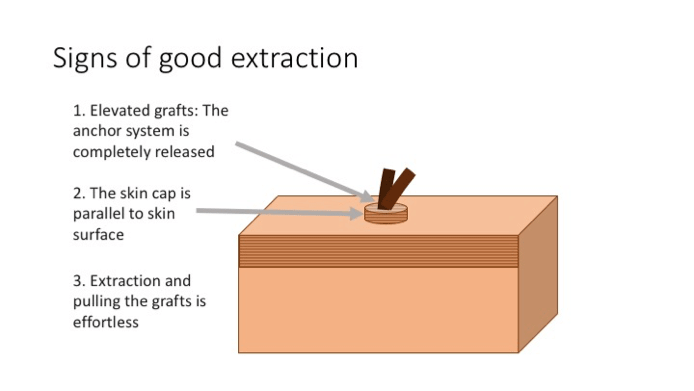
The surgeon should realize when the extraction is going well. Recognizing the following clues of a well-executed extraction will minimize unnecessary graft testing and reduce the overall technician pulling time. Positive extraction signs include:
- Grafts should be 0.5mm -1mm elevated – This means the anchor system is properly disengaged thus freeing the graft to allow for easy removal.
- Graft skin cap is parallel to the scalp – This usually indicates that the graft is properly scored and it would be unlikely that there is a partial or complete transection
- Effortless pulling of grafts by the technicians – Effortless pulling denotes proper scoring with correct depth. If there is any tethering the surgeon should increase the depth gradually to find the minimal depth required that will free the grafts from their anchoring points
Pulling Scored Grafts
- Two handed technique:
This is when the graft cap is grabbed in two steps:
- Step one: fine forceps provide the initial gentle upward lift. These fine forceps may be serrated or not depending on the case. If the graft is not naturally elevated, placing the forceps tip into the canal may be required to elevate and retrieve the graft.
- Step two: serrated forceps grab the graft below the first forceps (as low as possible along the graft), and pulls in a direction that is perpendicular to the direction of the forceps serrations. This perpendicular force applied with the 2nd forceps along with a deep grab will decrease the possibility of tethering.
If there is a problem with pulling the grafts, the technician should communicate this with the surgeon. Most common reportable issues include:
- Tethering: Resistance in pulling of the grafts aka tethering. This should be reported to the surgeon promptly as this implies the anchor system is not completely cut and the depth of scoring should be increased.
- Capping: Indicates that the grafts are not fully liberated. Continued pulling will only remove the top skin or cap. To remedy capping, the depth of scoring should be increased.
- Transection: Angle of scoring needs to be adjusted if transection occurs. Most transections occur as a result of an incorrect angle of approach or being off center when making the initial score. Partial transected grafts are of great value by providing feedback to the surgeon as to which direction to adjust the punch angle. The required angle adjustment depends upon the appearance of the partially transected graft.
- Off Center Grafts: A well scored graft should display a nicely centered hair. This minimizes the risk of partial or complete transection due to a slight deviation in the punch angle.
- Choice of forceps for a 2 step and 3 step extraction:
- For step one of the extraction, fine forceps can be serrated or non-serrated.
- In step two, a thicker tip with serrations allow for grabbing of the graft as deep as possible followed by a pull parallel to the skin yet perpendicular to the serrations.
- If there is resistance (tethering) during the two-step extraction, the serrated forceps releases and takes a second grab for the graft even lower as it reaches in to the hole before grasping and pulling perpendicular to its serrations. This last maneuver is called the 3rd step of extraction.
- Lastly, a circular jiggle is instituted with the serrated forceps to free the any remanence of the anchoring system which is still holding the graft in place. This is the “3 step plus”.